Table of Contents
Antibiotic resistance is rapidly becoming one of the most significant global health threats. While many people understand that overprescription of antibiotics by healthcare professionals contributes to this problem, fewer realize that everyday habits and choices play a major role as well. The routine decisions we make—whether it’s how we treat an illness, what we eat, or how we maintain hygiene—can either help combat or exacerbate antibiotic resistance. In this article, we explore how our daily habits contribute to the rise of antibiotic resistance and what we can do to minimize the impact.
Key Takeaways
- Global Crisis: Antibiotic resistance threatens public health worldwide.
- Daily Choices: Misusing antibiotics and poor hygiene contribute to resistance.
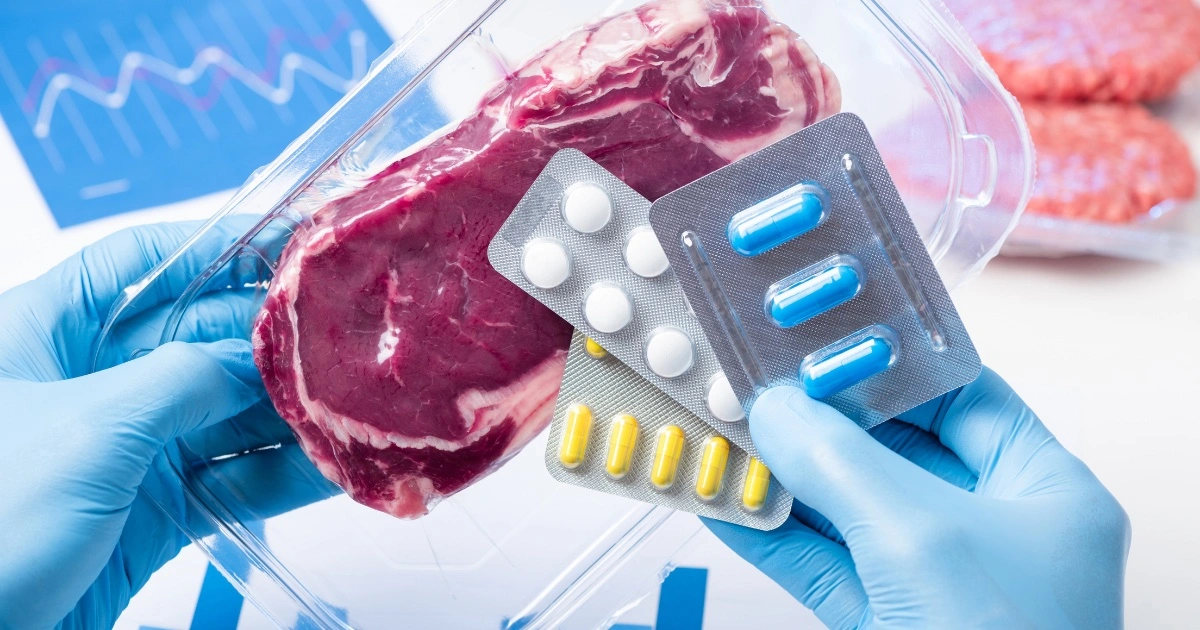
- Food Impact: Consuming antibiotic-treated meat spreads resistant bacteria.
- Healthcare Strain: Resistance leads to higher costs and prolonged illnesses.
- Take Action: Use antibiotics responsibly and support antibiotic-free products.
The Global Impact of Antibiotic Resistance
Before diving into how our behaviors contribute to this crisis, it’s important to understand the scale of the problem. Antibiotic resistance occurs when bacteria develop the ability to defeat the drugs designed to kill them. As a result, infections become harder to treat, leading to prolonged illnesses, higher medical costs, and increased mortality rates.
According to the World Health Organization (WHO), at least 700,000 deaths each year are attributed to antibiotic-resistant infections. If no action is taken, this number could rise to 10 million deaths per year by 2050. Antibiotic resistance has the potential to undo decades of progress in modern medicine, making once-treatable infections dangerous once again.
Daily Habits that Contribute to Antibiotic Resistance
While healthcare providers play a crucial role in the appropriate use of antibiotics, individual behavior also has a significant impact. The following daily habits are key contributors to the growing problem of antibiotic resistance.
Misuse of Antibiotics for Viral Infections
One of the most common ways people inadvertently contribute to antibiotic resistance is by using antibiotics for viral infections. Antibiotics are designed to treat bacterial infections, but many people mistakenly believe they will help cure viruses like the common cold, flu, or bronchitis. In fact, antibiotics are completely ineffective against viral infections, and using them unnecessarily only promotes resistance.
For example, the Centers for Disease Control and Prevention (CDC) reports that nearly 30% of antibiotic prescriptions in the United States are unnecessary, with many being written for viral infections that don’t respond to antibiotics .
Not Completing the Full Course of Antibiotics
Another harmful habit is not finishing the prescribed course of antibiotics. Patients often stop taking antibiotics once they start feeling better, but this can leave some bacteria in the body alive. These surviving bacteria are often the stronger, more resistant ones, and they can multiply, leading to a resistant infection.
Even if symptoms improve, it’s crucial to complete the entire course of antibiotics as prescribed by a healthcare provider. This ensures that all the bacteria are eliminated and reduces the risk of developing antibiotic-resistant strains.
Overuse of Antibiotics in Agriculture
The food we eat also plays a role in the spread of antibiotic resistance. In agriculture, antibiotics are often used not just to treat sick animals, but to promote growth and prevent disease in healthy livestock. This overuse of antibiotics in animals can contribute to the development of resistant bacteria, which can then be transmitted to humans through contaminated food or the environment.
According to the World Health Organization (WHO), antibiotic use in animals is one of the biggest drivers of resistance, and they have called for a global reduction in the use of antibiotics in agriculture, especially for growth promotion .
Overuse of Antibacterial Products in Daily Hygiene
In an attempt to stay clean and germ-free, many people use antibacterial soaps and hand sanitizers on a regular basis. However, the overuse of antibacterial products can contribute to antibiotic resistance by killing both harmful and beneficial bacteria. Some antibacterial agents, like triclosan, have been linked to the development of resistant bacteria.
The Food and Drug Administration (FDA) has banned triclosan in consumer antibacterial soaps, citing concerns over resistance and potential health risks. However, antibacterial products are still widely available, and their overuse remains a concern .
Poor Hand Hygiene
While antibacterial products can contribute to resistance, failing to maintain basic hand hygiene also plays a role. Inadequate handwashing can spread bacterial infections, leading to an increased need for antibiotics. According to the CDC, proper handwashing can prevent 30% of diarrhea-related illnesses and 20% of respiratory infections.
Poor hygiene practices allow bacteria to spread more easily, increasing the chances that someone will need antibiotics to treat an infection. Simple habits like regular handwashing with soap and water can help prevent the spread of infections and reduce the reliance on antibiotics.
The Role of Food in Antibiotic Resistance
What we eat is another key factor in the spread of antibiotic resistance. Here are two major ways that food and diet contribute to this global crisis:
Consuming Meat Treated with Antibiotics
Many consumers are unaware that the meat they eat may come from animals treated with antibiotics. When animals are given antibiotics to promote growth or prevent disease, resistant bacteria can develop in their bodies. These bacteria can then be passed to humans through the consumption of meat, dairy, or eggs. This can lead to antibiotic-resistant infections in humans.
To reduce this risk, it’s important to look for meat labeled “antibiotic-free” or “raised without antibiotics.” By choosing antibiotic-free options, consumers can support farming practices that don’t contribute to the spread of resistance.
The Impact of Overprocessed Foods
While antibiotics in animal agriculture are a major concern, overprocessed foods can also affect gut health and increase susceptibility to bacterial infections. Processed foods, which are high in sugar, salt, and preservatives, can disrupt the balance of the gut microbiome—the community of beneficial bacteria that plays a critical role in digestion and immune function.
A healthy microbiome helps protect against infections and reduces the need for antibiotics. Eating a balanced diet rich in fiber, fruits, vegetables, and probiotics can support a healthy gut and reduce the risk of antibiotic-resistant infections.
Consequences of Antibiotic Resistance on Public Health
The widespread misuse of antibiotics in daily life has profound consequences for public health. As antibiotic resistance grows, we face the possibility of returning to a time when simple infections were deadly. The following are some of the most significant consequences of antibiotic resistance:
Increased Mortality and Morbidity
Without effective antibiotics, common bacterial infections such as pneumonia, urinary tract infections (UTIs), and sepsis become more difficult to treat. As a result, infections last longer, are more severe, and may lead to death. According to the World Health Organization (WHO), infections caused by antibiotic-resistant bacteria lead to higher death rates than infections treated with non-resistant bacteria .
Prolonged Hospital Stays and Higher Healthcare Costs
Antibiotic resistance increases the burden on healthcare systems by prolonging hospital stays and requiring more intensive care for patients with resistant infections. This not only strains resources but also raises healthcare costs. In the United States, the CDC estimates that antibiotic-resistant infections lead to more than 2.8 million infections and over 35,000 deaths each year .
Threat to Routine Medical Procedures
Many routine medical procedures, such as surgeries, chemotherapy, and organ transplants, rely on antibiotics to prevent and treat infections. If antibiotic resistance continues to rise, these procedures will become riskier, and their success rates may decline. Infections that were once easily preventable could become life-threatening, complicating recovery and leading to higher mortality rates.
Steps to Reduce Antibiotic Resistance in Daily Life
While the problem of antibiotic resistance is complex, there are steps individuals can take to help slow its spread. By making conscious choices in our daily lives, we can reduce our impact on antibiotic resistance.
Use Antibiotics Responsibly
One of the most important things individuals can do is to only use antibiotics when they are prescribed by a healthcare professional and to take them exactly as directed. Avoid using antibiotics for viral infections like colds or the flu, and always complete the full course of treatment, even if you start feeling better.
Opt for Antibiotic-Free Foods
Choose antibiotic-free meat, poultry, and dairy products to reduce the demand for antibiotics in agriculture. Support farmers who use responsible practices, and look for labels that indicate no antibiotics were used in raising the animals.
Maintain Good Hygiene
Practicing good hygiene, including regular handwashing with soap and water, can prevent the spread of infections and reduce the need for antibiotics. This simple step is one of the most effective ways to avoid infections.
Avoid Unnecessary Antibacterial Products
Limit the use of antibacterial soaps and hand sanitizers, especially those containing triclosan. Regular soap and water are just as effective at preventing infections without contributing to antibiotic resistance.
Educate Yourself and Others
Raising awareness about antibiotic resistance is key to combating the problem. By educating yourself and others about the risks of antibiotic misuse and the importance of responsible practices, you can help create a culture of careful antibiotic use.
Conclusion
Antibiotic resistance is a growing threat that affects everyone, but the choices we make in our daily lives can help reduce its impact. From using antibiotics responsibly to supporting antibiotic-free farming practices, we all have a role to play in slowing the spread of resistance. By making informed decisions about our health, food, and hygiene, we can protect ourselves and future generations from the devastating consequences of antibiotic-resistant infections.
References
- Centers for Disease Control and Prevention (CDC). Antibiotic Resistance Threats in the United States, 2019. U.S. Department of Health and Human Services. https://ndc.services.cdc.gov/wp-content/uploads/Antibiotic-Resistance-Threats-in-the-United-States-2019.pdf.
- World Health Organization (WHO). Antibiotic Resistance: A Global Threat. WHO Publications, 2020. https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance.
- Ventola, C. L. (2015). The Antibiotic Resistance Crisis: Part 1: Causes and Threats. P&T Journal, 40(4), 277-283. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4378521/
- Laxminarayan, R., et al. (2013). Antibiotic Resistance—the Need for Global Solutions. The Lancet Infectious Diseases, 13(12), 1057-1098. DOI: 10.1016/S1473-3099(13)70318-9.
- U.S. Food and Drug Administration (FDA). FDA Issues Final Rule on Safety and Effectiveness of Antibacterial Soaps. https://www.fda.gov/news-events/press-announcements/fda-issues-final-rule-safety-and-effectiveness-antibacterial-soaps.
FAQ
- 1. What is antibiotic resistance?
Antibiotic resistance occurs when bacteria evolve to resist the effects of medications designed to kill them, making infections harder to treat. - 2. How do daily habits contribute to antibiotic resistance?
Everyday choices, such as misusing antibiotics for viral infections, not completing prescribed courses, and poor hygiene, can promote the development of resistant bacteria. - 3. Why is antibiotic resistance a global health threat?
The World Health Organization estimates that antibiotic-resistant infections cause at least 700,000 deaths annually, a number that could rise to 10 million by 2050 if not addressed. - 4. How can individuals help combat antibiotic resistance?
People can use antibiotics only when prescribed, maintain good hygiene, choose antibiotic-free foods, and educate others about the issue. - 5. What role does agriculture play in antibiotic resistance?
The overuse of antibiotics in livestock for growth promotion can lead to the development of resistant bacteria, which can be transmitted to humans through the food supply.